Still there is much frustration. It’s hard to get used to nurses not showing up to shifts, or showing up, but not bothering to give treatment to patients; It’s hard to accept when the hospital superintendent refuses to send an ambulance to transfer a critical patient, saying there is no money for fuel (or that it’s a waste of fuel to send a patient who might not reach Kampala); it’s infuriating to hear from a patient that a staff member demanded money from him for a service that should be provided for free; and it’s hard, very hard, when patients die due to improper care or a lack of a much needed drug, despite all efforts. It’s difficult not to feel responsible, even when we know (or at least hope), that we did everything possible.
Despite all the challenges, we feel we are making a significant change in the lives of many people. Despite resistance and a fair share of ego, we are trying to change working methods and customs, and to provide the staff with tools to deal with various problems given the local conditions. We are happy to report we found a volunteer couple who will arrive here in January and continue a few months after we head back home. We continue to look for volunteer doctors and nurses who will carry on the project. The need is great and we very much hope that funding will be secured and volunteers will continue coming.
Outreach in Kabuye

Two months ago we started our outreach clinic. The idea is simple – there is no health insurance in Uganda, and the distribution of government clinics is poor. Big towns have government health centers that are staffed, in the best case scenario, by a general doctor, and most commonly by a sort of physician assistant (called clinical officer). The mid-size and small towns have health centers staffed by a nurse, and the rural villages (where the majority of Ugandans live) have no health services at all. The great distances and rutted dirt roads make access to medical centers too far, too expensive, and not possible to a large part of the population.

We consulted the district health administration and various local health representatives and chose a village called Kabuye. Kabuye is located an hour and a half drive from Kiboga, on a rough road, far away from big and small health centers, in the middle of vast pasture land, in an area considered the district milk supplier. We loaded the car with boxes of medications and equipment, two loyal nurses, and set off on our way.

The first time we opened the clinic, we were swamped by a massive crowd. Dozens of people almost beat each other up to get in to see the doctors. We opened the clinic in a small, one-room shop belonging to the local priest, and tried (with partial success) to handle the masses. Later on we perfected the system, began to work in 2 rooms, added to our team a big-boned clinical officer, who does triage, hands out numbers to the patients (in an attempt to create an orderly line), performs HIV testing, and mainly prevents the human masses from trampling us. In the back room, we and the nurses examine the patients, dispense medications, and preform basic lab tests. There is a large variety of problems – many new HIV cases and other sexually transmitted diseases, various skin diseases, and numerous chronic problems that were never treated. At times the work is fascinating, at times exhausting, but we hope (and are already starting to feel) that going there and treating patients who have very poor access to medical care is important and beneficial.
Cherchez le boy…

A cute 2-year old boy named Junju arrives in the pediatric ward. He’s bad off, weighs only 8kgs, is coughing and struggling to breathe. We set out trying to find out what he suffers from and it is soon revealed that the kid has a huge abscess (infectious wound) in his lungs. It could be Tuberculosis or possibly another infection. After starting treatment, there was only mild improvement, and we were on the verge of transferring him to a larger hospital in Kampala.
The next morning Eitan arrives at the ward and discovers that Jungu is gone. His mom took him early in the morning and disappeared from the hospital. Eitan’s heart is broken thinking that Junju has joined the long list of lost patients who disappeared or went off to ‘witchcraft’.
And then came Grace, the in-charge nurse in pediatrics. Armed with Eitan’s promise to get a chicken if she succeeds in locating the boy, she sets off on a detective operation, questions all the parents in the ward, finds out who talked to the mother, collects information from here and there – and then declares – “We have a lead!! Where is the chicken?” After Eitan clarifies that she will get the chicken only after the boy is found, the two set off with a fighting spirit to the nearby village, where the lead says the kid’s grandmother lives. After going from house to house, the grandmother’s house is finally located, only to discover that Junju and his mom had been there this morning and had just left (‘chicken?’). After much convincing and a promise that we would not send them to Kampala (the mother ran away because she had no money to get to Kampala and was scared we will tell her to go), and with much help from the extended family, Junju was returned to the ward and continued treatment with marked improvement (‘chicken!!!’).
Ebola

Recently everyone who talks with us is interested in finding out if Ebola has reached Uganda. So, no. It is on the other side of the continent. It’s like asking if Israel has Japanese meningitis only because we and Japan are both in Asia. Despite the physical distance, the local medical staff is also a bit concerned. This is a global world and every bleeding patient is a potential suspect. A few weeks ago, during routine rounds in the women’s ward, one of the patients started to bleed. Not Ebola. No. Calm down. The nurses, on the other hand, didn’t calm down. In 5 seconds both nurses evaporated from the ward and left Reut alone with the patient. Later, one of them, still young and without children, explained that she ‘doesn’t want to die without a photocopy’… As a symbolic preventative act, Eitan started a new custom among hospital staff. Instead of the traditional (and oh so infective) handshake, everyone switched to ‘Bonga’ (banging fists), while declaring ‘Ebola’ or ‘TB’, depending on the mood.
Natural living
In the current atmosphere, when every doctor is accused of being a greedy gold digger and every vaccine is accused of containing mercury, we collected a few anecdotes about ‘natural’ living and the health that accompanies them. The weak hearted are advised to skip to the next section.

A 39 weeks pregnant woman is brought to the hospital after over 24hrs of labor at home with no progress – there are contractions, but the labor is not progressing. The labor was not delayed because of an epidural (because there is none), but because this is what happens in some deliveries. In western medicine, doctors look at their watch and when time is up (the risk of complications gets much higher when labor delays over a certain amount of time), they take the woman for a caesarian section (and are often accused of unnecessary intervention). When this woman came to Kiboga hospital, there were no doctor around to look at their watch, the nurses went to sleep, and in the morning the woman was found dead in her bed. They didn’t induce, they didn’t rush her to a C-section. ‘Natural childbirth’. (And also criminal negligence, but that’s a different story).
A newborn arrives in the pediatric ward. Only a week old. He was born in a regular and uneventful birth in a small ‘health center’, and was well and happy until a day prior to his arrival. Suddenly he deteriorated, stopped breastfeeding, and started convulsing non-stop. All clinical signs pointed to Tetanus, and in further questioning – we found that the mother had not been vaccinated during pregnancy (this is done in Uganda since not enough of the population is vaccinated against Tetanus). Yes, Tetanus. This weird, life threatening disease that you get vaccinated for in the west when you get a deep cut or an accident. A newborn can catch Tetanus through an infection in the umbilical cord and vaccination protects against it almost completely. The hospital doesn’t have the required treatment for the disease (which is only available in private pharmacies in Kampala, for a hefty sum). That same night the child died in Eitan’s hands.
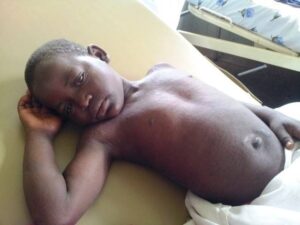
The same week (yes, when it rains it pours), another adorable girl was brought to the pediatric ward. Six-year old Joan came with signs of an infection in the brain (encephalitis) – impaired consciousness, confusion, with moments of clarity (in which she was very excited to see the white doctor and insisted on giving him a ‘bonga’ – the local high five). While examining her, Eitan noticed bite marks on her leg. It turns out that 3 months ago the child had been bitten by a stray dog, but didn’t receive a Rabies vaccine. She was sent to Kampala, confirmed as suffering from Rabies, and died after a few days. Rabies has a 100% death rate once clinical signs appear. Both Tetanus and Rabies are diseases found everywhere, even in Israel, and are effectively and safely prevented by vaccines.
So what are we trying to say? That sometimes there is much sadness and frustration here. That every day we appreciate what we have back home – the resources, the medications, the checks and balances that reduce mistakes and mistreatment. That we are amazed by the ‘health bubble’ that we are living in, in Israel and the rest of the western world, and are frustrated by those people who fail to understand that this ‘health bubble’ is delicate and fragile, and depends upon everyone’s cooperation with the health system.
Delegation from Israel
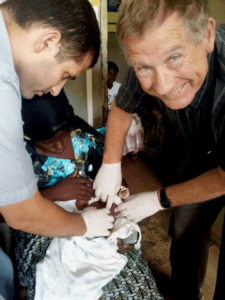
In September, Eitan’s parents came to visit for a full month. Danni, Eitan’s dad, who is a pediatrician and a specialist in infectious diseases, joined us in the hospital, gave first-hand consultations (and not through ‘WhatsApp’ as usual), hypnotized children (a well-known special ability of his…), encouraged us in tough moments, and got very mad at indifferent officials. We enjoyed very much working with him in the hospital and from the ability to consult with a senior and experienced doctor on a daily basis. We feel that he went back home with a better understanding of the medical world we are struggling with.

In the meanwhile Ruti, Eitan’s mom, opened a neighborhood day care and closed gaps with her grandson. There were many small and sweet moments with the family, but mostly we felt how they are becoming part of our life here. It’s hard to explain what life is like here, the rhythm is different, the terminology is different, the smells and weather are different. It was fascinating to see Danny looking at a critical patient, frustrated that we don’t have the means to care for him and he doesn’t have the money to go somewhere with better care; to watch Ruti panic because Eitan no longer stops when police officers signal him to stop because he’s fed up with them asking for a bribe every single time; to look at everyone gathering rain water into jerrycans, since there is no running water and we live from rain to rain, or working in the garden so there will be cucumbers for dinner. We felt that we have partners to our Ugandan life, that we are a bit more understood.
 |
 |







