In our last post we told you about our bureaucratic struggles, the long and tedious journey to get the needed papers and documents and arrange ourselves a place to live at. It was a hectic month,  but the house is standing and the neighbors are very nice – most of them are hospital staff and all are very welcoming. Every once in a while someone stops by to bring us avocado, maize or beans from their garden, and at the evening everyone sits outside and chats with us about Israel and the holy places, the food we eat back home, how children are raised and of course – what the hell is a Jew and which church do we attend… And of course, our house is surrounded by many cows, chickens, turkeys, dogs and goats (some of them decided that staying inside our house is even better…).
but the house is standing and the neighbors are very nice – most of them are hospital staff and all are very welcoming. Every once in a while someone stops by to bring us avocado, maize or beans from their garden, and at the evening everyone sits outside and chats with us about Israel and the holy places, the food we eat back home, how children are raised and of course – what the hell is a Jew and which church do we attend… And of course, our house is surrounded by many cows, chickens, turkeys, dogs and goats (some of them decided that staying inside our house is even better…).
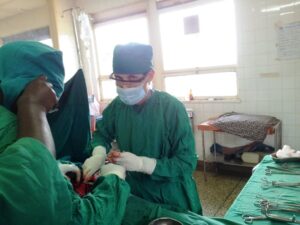
While Eitan continues to single handedly manage the ‘renovation’ and countless other tasks, Reut started working in the hospital, at Maternity ward.
Where do we even start telling you about this crazy hospital? Let’s start by saying that we will never (never!) again complain about the wonderful health system in Israel…
Kiboga hospital has 120 bed, divided into 4 wards – maternity, pediatrics (children), female and male (the last two act as internal & surgical departments). In addition there is an outpatient department, also acting as an emergency room, antenatal, HIV & tuberculosis clinics. We were told that there are 4 doctors working in the hospital. Well… no. In realty there is one doctor on-call at any given time, and the others are off in the capitol working in private clinics or farming… Yes, one doctor on a hospital of 120 beds plus an active emergency room (Just to clarify, in Israel there would be over 50 doctors in a hospital this size). One of the doctors working in the hospital is a gynecologist, and the others are general practitioners, without a specialty. General practitioners do everything here – working in all the wards, handling trauma cases, preforming caesarian sections and what not.
Since there is only one doctor around, the wards are run by the nurses – usually one nurse on an entire ward of around 30 patients. Patients arriving at the emergency room are seen by a clinical officer (‘half’ a doctor with 3 years of training) or a nurse, who takes the history (and rarely has time to do a physical examination) and do some very basic lab tests, admit the patient and decide on a treatment. The wards are run by the nurses – usually one nurse on an entire ward of around 30 patients. The one doctor in the hospital spends most of his time in the operation room, performing caesarian section, and handling obstetrical emergencies.
There are no doctors rounds in the wards, and the patients just lay there, get their medications (only if they are lucky, since many times the drugs run out of stock, the key to the medicine cabinet is missing, or the nurse just didn’t have the time), and either get better or not… No one examines them again, sees if the initial diagnosis was correct or if the treatment needs to be changed. The doctor is called only when there is an emergency (and only if the nurses noticed that there is an emergency…), or when the patient needs an operation.
The physical conditions are very different from those we are familiar with (you complain about 4-5 patient’s in a room…? Please!). Each ward is one big room, where patients lay all together (including tuberculosis patients and other highly infectious diseases…), without curtains or any form of privacy. All examinations are conducted in the same room, and only when a very intimate examination or procedure is preformed someone bothers to bring half-a-curtain that half-covers-something…
For the past 8 (!) years there is no running water in the hospital (since the pump supplying water from the lake is broken), and even scrubbing for an operation is done with water from a jerrycan (with mud at the bottom).
Power is not always on and fuel for the generator is not always available. This means that the lab occasionally works, and same goes for the light in the operation room and the oxygen generator. It’s all a matter of luck. The various machines, such as lab equipment, oxygen, X-ray & even blood pressure machines are on rotating duty as ‘broken’, ‘missing parts’ and ‘no one to operate’. The same goes for the operation room, where you have to suite up with a butchers apron & fishermen’s boots, since the suction machine (the one that suctions the blood during operations) retried due to old age, and the patients are put to sleep using ‘ether’ gas (which has not been used in the west for decades since it’s dangerous to the patient, highly flammable and gets the anesthesiologist stoned…) although at the side of the room stands shyly a brand new ventilation machine that uses modern gasses (this one is on ‘missing parts’ duty).
The supply of drugs is very limited and many times we have to give medications that are not optimal since nothing else is available, or we happen to find out (usually by chance) that the patient hasn’t received his meds since it ran out of stock. The treatment in government hospital is supposed to be provided for free, but in many cases patients are sent to buy drugs that are missing (or even a surgical blade…), and are expected to provide for many things themselves (such as food, bed sheets, gloves etc…). Some tests (such as ultrasound) are not available at the hospital and patients are sent to a private clinic (for full payment). Every day we see patients that can’t afford a drug or a test they require. Even when you decide a patient is too complicated and must be transferred to a bigger hospital, you are again confronted with a challenge – the ‘ambulance’ taking the patient is in fact a van with only a driver and no medical staff or equipment. More often than not, the family is asked to pay for the fuel (an astronomical amount for many). The cost causes many patients to refuse transfer even in critical cases, or at the best case, choose to go by public transportation.
Maternity is the busiest ward in the hospital. The two midwifes on shift are in charge of the ward, the delivery rooms and the operation room. The on-call doctor arrives only when there is an emergency, or a need to perform a caesarian section. Reut started doing doctor rounds, attending to complicated cases in the delivery room and joining operations. The antenatal care and delivery management is somehow different than in Israel (where pregnant women see their doctors more than their husbands, and go through countless tests and examinations)… Here most women who come to deliver don’t really know which week they are on, their antenatal care consisted of 0-2 visits to a midwife, with no ultrasounds or visits to a doctor. The delivery room is also far off from those in Israel. All of the women are waiting to deliver in one room (some on a bed and some on the floor). A ‘fetal heart monitor’ is actually a midwife that comes around once every few hours to examine the woman and listen to the baby’s pulse with a ‘fetoscope’ (a metal tube which is placed on the belly while the midwife presses her ear to the other side). Only at the very last stage the woman is moved to a bed with a curtain, to push the baby out in private. In the end everything is cleaned with bleach (including the new mother), and the next in line is immediately brought in.
The Ugandan pace is extremely slow and even in emergencies. The midwifes take forever to call the doctor or move the patient to the operation room. The newly born babies are not routinely monitored by the staff. They stay in the same bed with their mother, who is supposed to report if something is wrong. With all this, combined with the poverty, the living conditions, the limited access to medical care and the prevalence of infectious diseases, it’s not surprising that the complication rate and infant mortality are very high. The attitude towards death here is almost nonchalant. A normal part of every-day life. Even when a 19 year old loses her first born child during delivery, the mother is almost casually told, there is no crying, no screaming. This is life. You move on. Despite the conditions and the challenges, there are also many success stories, when lives are saved after severe complications during childbirth.
Two weeks after Reut and after triumphing over the bureaucracies and fixing all (or at least most) of the problems in our house, Eitan started working in Pediatric (children) ward. Upon arrival in the ward on the first day he saw the ward was packed and asked when are the round. He was told ‘good you’re here, lets start’. He suggested they wait for the doctor in charge, and was told ‘you are the doctor in charge’. And so the day began…
The ward is very busy with many children suffering from severe malaria with various complications, many children with ‘viruses’ just like in Israel (that are also treated for malaria, just in case), as well as quite a few children with severe malnutrition. Plenty of work to go around. The issue of money and parental priorities is ever present. Many times you wish to refer a complicated case to a bigger hospital in the capital, but the parents decide to go back home, since they don’t have money for transport or for food while in the hospital, even when they know that this means their kid is going to die – such as the case of a two year old with a congenital heart problem or a three year old after a severe head injury with intracranial bleeding. Another difficult challenge is reaching a diagnosis and providing adequate treatment, when the limited resources and lack of power limit the options. In many cases Eitan finds himself running around the hospital trying to get the generator turned on, so that an unconscious child can get oxygen, and necessary lab tests can be done.
The work is very challenging, especially since we are only beginning our professional career. The diseases are completely different than the ones we know from home and diagnosis is done mainly using a history & physical examination, and not much else. With all that in mind, we are slowly coming to realize that we have much to contribute. Since there is only one local doctor in the hospital at any given time and he is usually spending all his time in the operation theater – there are zero doctors taking care of all the other patients. This is where we come in. We do doctor rounds at the wards, see the patients and follow up on them (what would not have been done at all if we weren’t here). Many times we find that the initial diagnosis was far from on the mark (most patients are automatically diagnosed with malaria, even if the patient actually suffers from pneumonia, a skin infection or even a head injury…). We still have a lot (a lot!) to learn in medicine in general and in tropical medicine specifically, but we see the patients, follow up, adjust the treatment, consult other doctors (local ones or our panel of loyal consultants from Israel via whatsup). All the things, which would never have happened, simply because there are not enough doctors in the hospital.
Every day we come to appreciate more the Israeli health system, with the vast number of professional staff, the resources that seem to be almost unlimited from here and the work protocols which are strictly followed.
So apart from working in the hospital we managed to do a bit of traveling around Uganda – we visited a beautiful rhino reservation, where you can walk up close to see the rhinos, we walked around Budongo forest – a real jungle with baboons, birds, butterflies and giant trees. We also spent a quiet weekend in Entebbe, the first weekend where we really had the time to rest and weren’t busy with countless errands. And Eyal? It seems that he has already gotten used to the new house and to his lovely nanny. He spends his time walking around the town and playing with the neighbors kids. He babbles all the time and every day surprises us with a new word (half in Hebrew and half in Luganda), runs everywhere instead of walking and drives around the house in his toy-car, while yelling ‘vrum vrum!’.
So what’s next? We are currently spending a few weeks working in each ward, in order to get to know the hospital and the local medical practice, and to find out where we are needed most. We are also starting to organize the outreach clinic – where we will take a car, a large box of meds & equipment, a nurse and a translator and go to remote villages in the district that don’t have access to medical facilities (which is most of the district). Later on we plan on dividing our time between working in the hospital, where we feel we are making a difference, and going out to do outreach clinics. A little more in the future we plan on starting to build training programs for the local health staff such as nurses and clinical officers. In the meanwhile, we are also trying to establish continuity to this project and make sure we are followed by more volunteers that will continue are work.
All the best,
Eyal, Eitan & Reut